Technical Info
NIOSH stopped collecting data after 2023. This site will continue to be maintained but additional years of data will not be added.
Important Note
- 2011 to 2012 is a series break. Comparisons of injury events and sources should not be made between years that cross this break.
-
2014 to 2015 is a series break related to inclusion/exclusion of nonwork-related illnesses. Caution should be taken when comparing estimates of total cases between years that cross this break.
- 1998-2014 NEISS-Work data include illnesses that began at work (e.g., heart attacks and strokes), chronic conditions, and exacerbations of long-term injuries. These cases, classified as "illnesses," represent 5-10% of total annual case estimates.
- 2015-2023 data do not capture nonwork-related illnesses. See case exclusions for details.
-
2017 to 2018 is a break related to the available detail for event, source, and secondary source.
- Event, source, and secondary source for 2018-2023 data are only be available at one- and two-digit code levels.
- This change is due to the use of a machine-learning model to assign two-digit event and source codes to each case based on OIICS v.2.01.
Data Source, Design, & Case Definition
Estimates & Errors
Data Elements & Reports
- Treatment year
- Treatment month
- Age group
- Sex
- Race and Ethnicity
- Diagnosis
- Part of body affected
- Disposition of patient
- Event or exposure
- Source of injury
- Secondary source of injury
- Data reports
- Minimum reporting requirements
- Limitations
- Disclaimer
Data source
Work-RISQS is an online data access system for NIOSH surveillance data on nonfatal work-related injuries and exposures treated in U.S. hospital emergency departments (EDs). NIOSH collaborated with the U.S. Consumer Product Safety Commission (CPSC) to collect these data through an occupational supplement to the CPSC National Electronic Injury Surveillance System (NEISS) that does not require consumer product involvement. This occupational supplement is known as NEISS-Work. The NEISS-Work data were collected from 1998-2023.
Top of PageSample design
NEISS-Work was a national stratified probability sample of hospitals in the U.S. and its territories that have a minimum of six beds and operate a 24-hour emergency department (ED). Hospitals in the sample were selected from the approximately 5,300 rural and urban U.S. hospitals after stratification by total annual ED visits. The occupational injury hospital sample was a 2/3 subset of the hospital sample used by CPSC prior to 2023 to capture product-related injuries. Nominally, 67 geographically distributed sample hospitals captured work-related injuries every day of the year. Hospitals abstractors captured all treated cases that were identified as work-related, and coded case information from the medical record.
Each case was assigned a statistical weight based on the inverse probability of selection. National estimates are obtained by summing weights for all cases or the selected set of cases. Statistical weights were adjusted within a sample year to account for hospital mergers, closings, or withdrawals from NEISS-Work (resulting in fewer than 67 hospitals reporting information), and for incomplete reporting. Statistical weights were adjusted annually based on the number of U.S. hospitals and their total number of ED visits as determined by a census of U.S. hospitals one year prior to the data year.
Top of PageCase definition
NEISS-Work cases used for Work-RISQS estimates involved nonfatal work-related injuries and exposures among civilian, non-institutionalized workers, treated in the emergency departments of participating hospitals. Workers were not restricted by age, employer size, or type of employer or industry. An injury was considered work-related if the patient was working for pay or other compensation, performing agricultural production activities, or volunteering with an organized group (e.g., a volunteer fire department).
Top of PageCase exclusions
The following types of cases are excluded from NEISS-Work data:
- Injuries to active-duty military (Air Force, Army, Coast Guard, Marines, National Guard, Navy, or Reserve Officers' Training Corps [ROTC])
- Injuries of institutionalized persons, such as those in prisons or psychiatric institutions
- From 2015-2023 on, nonwork-related illnesses were excluded. Illnesses that remain in the data (e.g., dermatitis, asthma exacerbations, heat exhaustion) have documented links to work-related exposures. Prior to 2015, most illnesses that happened at work (excluding common illnesses such as colds and flus) were included.
- Drug and alcohol screenings
- Revisits to EDs for injuries previously treated in EDs
Case identification
Hospital abstractors identfied work-related cases from admissions information and emergency department chart review. NEISS-Work did not require a workers' compensation claim for inclusion.
Top of PageInjury estimates
NEISS-Work was designed to produce national estimates and is not suitable for regional, state, or local injury estimates. Extrapolating the number of cases seen in the approximately 67 hospitals by using the statistical weight of each case produces a national estimate. The statistical weight varied depending upon the size of the hospital and the number of patients typically treated in its ED. Each case captured in a sample hospital may represent from 20 to more than 100 cases seen in other U.S. hospitals. Summing the weights for similar cases gives a national estimate for all injuries, or for a specific demographic group, type of injury, or injury circumstance. In Work-RISQS, national estimates are expressed in thousands of injuries for a given year. For example, in 2022 there were an estimated 2,322.1 thousand (2,322,100) occupational injuries and exposures treated in U.S. hospital EDs.
Top of PageInjury estimate confidence interval
Because the NEISS-Work system was a sample of hospitals and did not count every injury treated in every hospital, the national estimates may be in error. However, because this sample was statistically selected, Work-RISQS can calculate the potential error. Error estimates are based on the 95% confidence interval and are expressed as a value that should be subtracted from the estimate to get the lower confidence bound and added to it to get the upper bound. For example, in 2022, there were an estimated 2322.1 thousand work-related injuries and exposures with a 95% confidence interval of ±7546.1 thousand cases. In other words, the true value from this system is likely to be in the range of 1,776,000 to 2,868,200 injuries and exposures, treated in U.S. EDs in 2022.
The 95% confidence interval is an approximation based on the classical formula for variance of a total from a stratified sample. The confidence bounds are approximations of the general magnitude of error regarding estimates, and are not precise values.
The variance estimating formula currently used by Work-RISQS is:
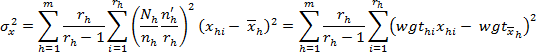
Where:
-
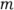 = Number of strata in the sample during the given time period
= Number of strata in the sample during the given time period -
 = Number of hospitals in the sampling frame for stratum h
= Number of hospitals in the sampling frame for stratum h -
 = Number of hospitals selected for the sample for stratum h
= Number of hospitals selected for the sample for stratum h -
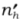 = Number of in-scope hospitals in the sample for stratum h
= Number of in-scope hospitals in the sample for stratum h -
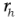 = Number of hospitals participating in stratum h for the given time period
= Number of hospitals participating in stratum h for the given time period -
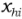 = Number of occupational cases for a specific type of injury reported by hospital i in stratum h for the given time period
= Number of occupational cases for a specific type of injury reported by hospital i in stratum h for the given time period -
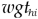 = Weight of hospital i in stratum h
= Weight of hospital i in stratum h -
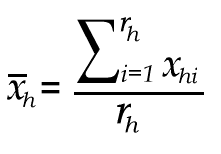
-
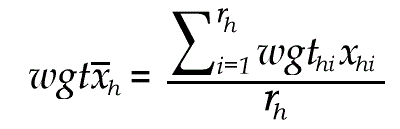
The 95% confidence interval, expressed as an amount to be subtracted or added to the national estimate, is then calculated as:
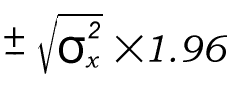
Where:
-
 = Variance of the injury estimate x
= Variance of the injury estimate x -
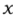 = Injury estimate
= Injury estimate
To minimize issues with negative variances,
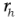 is calculated as a fractional
is calculated as a fractional
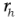 value where
value where
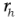 equals the sum of the number of months that all hospitals within a strata reported during the calendar period divided by 12 months.
equals the sum of the number of months that all hospitals within a strata reported during the calendar period divided by 12 months.
The confidence interval does not account for biases (nonsampling error) in the estimates that arise from the way in which data were collected or defined, the ability to identify all work-related cases, or mistakes in data collection or coding.
Top of PageWorker population
Work-RISQS numbers were derived from the NEISS-Work population: civilian, non-institutionalized workers of all ages and all employer or industry types and sizes.
To calculate a meaningful rate, the estimate for the selected worker population (denominator) should be the best possible match available for the Work-RISQS estimate (numerator). Users can obtain employed worker population estimates from the Employed Labor Force (ELF) query system. See How to Calculate Rates in the Work-RISQS Help section for more information about options for selecting a population in ELF.
Certain volunteer workers are included in the Work-RISQS injury counts. This creates an insignificantly small bias in rate estimates when the denominator population does not include volunteers.
Top of PageTreatment year
Definition: Calendar year in which the patient first received medical treatment in an emergency department for the injury.
Users may query injuries according to the date of first treatment in an ED, for one calendar year at a time, beginning with 1998 through 2023. Users cannot query multiple years simultaneously.
Top of PageTreatment month
Definition: Calendar month or quarter of year in which the patient first received medical treatment in an emergency department.
Users may select one or more months or quarters for queries. The months or quarters do not need to be consecutive. Injury estimates are based on the actual number of cases treated within the selected calendar month(s).
Top of PageAge group
Definition: Inclusive range of ages of patients (in years).
Injured workers are grouped by age ranges (primarily five-year ranges). Users may select one or more age groups. Age is unknown for a small proportion of cases. There are no age restrictions for cases captured in NEISS-Work.
Top of PageSex
Data for 2021-2023:
Definition: The distinction between male, female, and non-binary/other.
A worker's sex was reported in hospital data as “Male,” “Female,” “Non-binary/other,” or “Not Recorded/Unknown.” In any given year's data, the number of cases for which sex was “Not Recorded/Unknown” is very small (typically < 0.01% of all cases). Sex parameters for queries are All, Male, and Female; users may select only one per query.
Data prior to 2021:
Definition: The distinction between male, and female.
A worker's sex was reported in hospital data as “Male,” “Female,” or “Not Recorded.” In any given year's data, the number of cases for which sex was “Not Recorded” was very small (typically < 0.01% of all cases). Sex parameters for queries are All, Male, and Female; users may select only one per query.
Top of PageRace and Ethnicity
Data for 2019 onward:
Beginning with the 2019 data, race and ethnicity were separated into two variables. While this should be considered a break in series, it is possible to combine race and ethnicity to create groupings like those used prior to 2019.
Definitions:
- Race classifies people with similar biological, social, and cultural heritage into racial groups (White, Black, American Indian/Alaska Native, Asian/Pacific Islander, and Other) according to information in the ED chart.
- Ethnicity is coded as Hispanic when the ED record indicates the patient is Hispanic, Latino/Latina, or of Spanish origin. Hispanic Ethnicity includes people of Cuban, Mexican, Puerto Rican, South or Central American, or other Spanish culture or origin regardless of race.
Race was collected in two parts in the data. In the first part, hospital abstractors select "White," "Black/African American," "Asian," "American Indian/Alaskan Native," "Native Hawaiian/Pacific Islander," "Other," or "Not stated" for race. The second part was a free text field, where abstractors specifically describe races coded as "Other." Race and ethnicity are not always uniformly reported because NEISS-Work hospitals did not collect race and ethnicity data the same way, if they collected or reported it at all.
Data prior to 2019:
For data prior to 2019, race and ethnicity were combined into one variable.
Definition:
- The combined race/ethnicity variable classifies people with similar biological, social, and cultural heritage into racial groups (White [non-Hispanic], Black [non-Hispanic], American Indian/Alaska Native, and Asian/Pacific Islander) and one ethnic group (Hispanic), according to information in the ED chart.
Race and ethnicity were collected in two parts in the original data. In the first part, hospital abstractors select "White," "Black/African American," "Asian," "American Indian/Alaskan Native," "Native Hawaiian/Pacific Islander," "Other," or "Not stated" for race. The second part was a free text field, where abstractors more specifically describe races coded as "Other" or note ethnicity (such as "Hispanic" or "Latina"). Race and ethnicity were not always uniformly reported because NEISS-Work hospitals did not collect race and ethnicity data the same way, if they collected or reported it at all, and because of the manner in which race and ethnicity are captured in the NEISS-Work data. For example, a Hispanic patient might have been indicated in NEISS-Work as: (1) "White" or "Black" with a blank free text field (only race reported); (2) "White" or "Black" with "Hispanic" entered in the free text field (both race and ethnicity reported); or (3) as "Other" with "Hispanic" in the free text field (only ethnicity reported).
Work-RISQS recoded race and ethnicity under a single combined data structure, designated Race/ethnicity. Within this structure, Hispanic ethnicity was indicated preferentially over either White or Black race, so that workers identified in hospital records as "White" or "Black" and "Hispanic" or "Latino/Latina" were recoded as Hispanic.
Diagnosis
Definition: The nature of the most severe injury as described by the attending physician or other medical staff. If a medical diagnosis was missing from the ED record, the Diagnosis is typically the patient’s chief complaint.
The diagnosis categories used by NEISS-Work hospital abstractors were condensed into 25 categories for Work-RISQS queries. Categories with few cases (e.g., “Burn: electrical” and “Burn: not specified”) were combined into a larger reportable group (e.g., Burn: other). Diagnoses of "Ingested foreign object," "Aspirated foreign object," "Dental injury," "Other," and "Submersion" were combined in Other, n.e.c.
The coding of specific injury types may not always have been uniform because of ambiguous terminology and multiple diagnoses listed in the ED record. For example, two workers in different cities may strain their arms while lifting crates. One ED chart may note this as “patient strained arm,” coded as Strain or sprain, while another chart may describe the case only as "patient presented with arm pain,” coded as Other, n.e.c. To the extent it was possible to do so, these types of issues were minimized in the data.
Definitions of individual diagnoses typically followed standard medical usage. Anoxia, and Poisoning have specific definitions to help distinguish particular injuries:
- Anoxia was used when the patient could not obtain sufficient oxygen, due to hampered breathing or lack of oxygen in the breathable atmosphere. For example, this category was used when the diagnosis is strangulation, suffocation, or asphyxia; or when the patient has inhaled products of combustion such as carbon monoxide (CO), smoke, or soot.
- Poisoning is used when a patient swallowed liquid or soluble chemicals, drugs, or medications; inhales vapors, fumes, or gases (other than carbon monoxide, smoke, or other products of combustion, in which case the Diagnosis was Anoxia instead of Poisoning); or reacts systemically to a product absorbed through the skin.
Part of body affected
Definition: The region or part of the body most seriously harmed.
The part of the body primarily or most severely affected by the injury wwas the one coded. However, the injured body part may overlap two coding categories, such as a laceration to a finger and palm, which one hospital abstractor may have listed as “Finger” and another as “Hand.” Similarly, an injury to the eye may be coded as “Eyeball” or “Face” depending upon the information provided and the wording in the ED chart. Users should be cautious when comparing Work-RISQS estimates of body parts to adjoining body parts and when interpreting estimates of a specific part within a larger body region. Certain injury types have coding rules to minimize this issue:
- Back injuries were coded as Upper trunk when the was injury was above the waist or navel, and Lower trunk when below. A diagnosis of unspecified "back injury" was coded as Upper trunk.
- Burn injuries involving less than 25% of the body were coded as the most severely burned body part. More extensive burn injuries were coded as 25 to 50% of the body or All parts of the body (i.e., more than 50% of the body).
- Eye injuries were coded as “Eyeball” when the injury occurred directly to the eye itself, whereas injuries to the eyelids, eyebrows, or the area immediately around the eyes were coded as Face.
- Facial injuries were unspecified or more generally involved a broader extent of the face were classified as Face even though there may have been damage to one or both eyes or to the mouth.
- Head injuries with general diagnoses of "head trauma," "closed head injury," or "blunt head injury,” instead of a specific diagnosis such as “Laceration” or “Concussion,” were coded as Internal organ.
- Injuries with diagnoses of Anoxia, Electric shock, Poisoning, or “Submersion” were coded as All parts of the body.
- When the diagnosis was “Aspirated foreign object” or “Ingested foreign object,” the Part of body is coded as Internal organ.
Disposition of patient
Definition: The status of a patient after treatment in the ED, categorized as Treated and released, Treated and transferred/hospitalized, or Unknown.
About half of Treated and transferred/hospitalized patients were hospitalized in the same facility as the ED. The other half were transferred to a different facility, generally a specialty-services hospital (e.g., burn center or pediatric hospital) or other higher-level care facility. Many of the transferred patients were hospitalized in the new facility, but their final disposition was not always known.
Top of PageEvent or exposure
Definition: The manner in which the injury was produced or inflicted, as coded in the BLS Occupational Injury and Illness Classification System (OIICS).
The Event or Exposure was classified in a hierarchical structure with general divisions of aggregate single-digit codes that narrow into more specific categories with two-, three-, and four-digit codes. Aggregate categories, which are identified by asterisks after the code digits (such as 2* or 63*), include all subcategories and individual codes listed below the aggregate category.
Analysis of more detailed codes may not produce reportable results because the selected Event may have occured only rarely, or because a lack of description in ED records may not have allowed for more detailed codes. For example, using OIICS v2.01, a case in which a worker fell seven feet off the edge of a loading dock to the ground below would be coded as 4332 Other fall to lower level 6 to 10 feet if the abstractor provided that level of detail in the final NEISS-Work data. However, the same injury might be described in the ED chart simply as "fell at work." In that instance, the Event would have been coded as 420 Fall on same level, unspecified (the default when the height of a nonfatal fall is unknown), or 430 Fall to lower level, unspecified (if the severity of the resulting injuries suggested a fall from elevation). Injury estimates for specific Events may therefore significantly underestimate the true number, and should be considered minimum estimates.
Note that data years 1998-2011 use BKS Occcupational Injury and Illness Classification System(OIICS) v1.01 for Event, Source, and Secondary Source, and data years 2012-2023 use OIICS v. 2.01. The query system defaults to the appropriate version based on the year selected. There is a break in series between the versions, and users should not compare Event, Source, and Secondary Source results between years that use different versions (e.g., 2011 and 2012).
For data years 1998 through 2017, each case was manually coded to the most specific level of detail (two-, three-, or four-digit codes) possible by a trained coder using information abstracted from the ED record.
Starting with data year 2018, event or exposure was coded using a machine-learning model to assign OIICS two-digits event or exposure codes to each case. The model predicts event or exposure codes based on the narrative description of the injury and the worker's age and sex. Event or exposure codes that do not meet specified threshold scores, reflecting the certainty at which a code was assigned, were flagged for review by a trained coder.
Top of PageSource of injury
Definition: The object, substance, person, bodily motion, or exposure which directly produced or inflicted the injury, as coded in the BLS Occupational Injury and Illness Classification System (OIICS).
Source, like Event, was classified in a hierarchical structure with general divisions of single-digit codes that narrow into more specific categories with two-, three-, and four-digit codes. Aggregate categories, which are identified by asterisks after the code digits (such as 2* or 63*), include all subcategories and individual codes listed below the aggregate category. As with Event, the more detailed levels may not produce tables with reportable results because the selected Source may only rarely appear in NEISS-Work cases, or because a lack of description in ED records may not allow for more detailed codes.
There are far more codes available for Source than Event because of the diversity of objects, substances, environments, and exertions that can produce injury. For example, using OIICS v 2.01, if a worker was struck in the eye by a flying nail, the Source code would be 4212 Nails, brads, tacks, nuts, bolts, washers. Other fasteners (e.g., rivets, screws, and staples) each have separate 4-digit source codes. As for Event, estimates of specific Sources were difficult to consistently identify and should be considered minimum estimates.
As with Event, the query system defaults to the appropriate version of OIICS based on the year selected. There is a break in series between the versions, and users should not compare Event, Source, and Secondary Source results between years that use different versions (e.g., 2011 and 2012).
For data years 1998-2017, each case was manually coded to the most specific level of detail (two-, three-, or four-digit codes) possible by a trained coder using information abstracted from the ED record.
Starting with data year 2018, was coded using a machine-learning model to assign OIICS two-digit source codes to each case. The model predicts source codes based primarily on the narrative description of the injury and the worker's age and sex. Source codes that do not meet specified threshold scores, reflecting the certainty at which a code was assigned, were flagged for review by a trained coder.
Top of PageSecondary source of injury
Definition: The object, substance, or person that generated the source of the injury or that contributed to the event or exposure, as coded in the BLS Occupational Injury and Illness Classification System (OIICS).
The Secondary Source was classified using the same structure and with the same codes as the Source. An example of a secondary source would be a tool that set into motion a flying object which then struck a worker. If the worker noted above who was injured by a flying nail was hammering the nail at the time, the hammer would be the secondary source. Another example of a secondary source would be spilled water that caused a worker to slip and fall to the floor.
About 80% of cases have no Secondary Source coded, either because the lack of description in a record prevented identification of a secondary source or because there simply was no secondary source for that case.
For data years 1998-2017, each case was manually coded to the most specific level of detail (two-, three-, or four-digit codes) possible by a trained coder using information abstracted from the ED record.
Starting with data year 2018, event and primary source codes were assigned via machine learning. However, machine learning could not be used to assign secondary source codes. Thus, two-digit secondary source codes were applied by a trained NIOSH coder for select events: intentional injury by person (11), falls on same level (42), exposure to other harmful substances (55), and struck by object or equipment (62).
Top of PageData reports
A Work-RISQS query results in a table of national injury estimates. Each table lists the query parameters selected for that particular estimate and the results of the query. The table columns include a national estimate (in thousands), the confidence bounds (in thousands) expressed as a value to be added to and subtracted from the national estimate to give the 95% confidence interval, and the percentage of the total estimated injuries for the year.
Top of PageMinimum reporting requirements
Work-RISQS uses three criteria to determine if a national estimate is reportable. First, estimates must be based on a minimum number of cases among the small sample of U.S. hospitals within NEISS-Work. Second, the national estimate must exceed a minimum number of injuries. Third, the error associated with an estimate must be small enough to indicate that the estimate would be reasonably reproducible (i.e., the coefficient of variation is less than or equal to 30%). To be reportable, a national estimate must meet all three criteria. Work-RISQS automatically verifies that results meet the reporting requirements.
Top of PageLimitations
NEISS-Work data have several limitations that should be considered when interpreting and reporting results. First, 1998-2011 NEISS-Work data use OIICS v.1.01 for event and source codes. NEISS-Work data from 2012-2023 use OIICS v.2.01. Comparisons between event and source should not made between years that cross this break. Second, 1998-2014 NEISS-Work data include nonwork-related illnesses that began at work (e.g., heart attacks and strokes), chronic conditions, and exacerbations of long-term injuries. These cases, classified as “illnesses,” represent 5-10% of the total estimates for these years. NEISS-Work data from 2015-2023 did not capture most nonwork-related illnesses. Caution should be taken when comparing estimates between years that cross this break. Third, the small number of hospitals in the NEISS-Work sample contributes to large confidence intervals. Fourth, NEISS-Work data represent only injuries treated in EDs, omitting injuries treated in other medical venues and self-treated injuries. Finally, case capture relies on information found in the ED medical record identifying the case as work-related, and inaccuracies may occur due to the lack of information provided by the worker, incomplete medical records, or errors in abstracting the information from the record.
Top of PageDisclaimer
Although NIOSH extends considerable effort to ensure reasonable data quality for Work-RISQS estimates, there are no warranties expressed or implied with these data. The underlying data for queries are subject to change without notice as errors, inconsistencies, or other data issues arise. The objective of Work-RISQS is to provide public access to occupational injury data for use in workplace-safety and injury-prevention activities where understanding the general magnitude of injuries, worker characteristics, and injury events is important. Use of these data for other purposes should be done with caution.
Top of Page